Archives: Pillars


“Hiding in the nucleus, in plain sight, wreaking havoc,” is how Paul S. Mischel, MD, a long-time member of the American Association for Cancer Research (AACR) and a Fellow of the AACR Academy, characterizes the circular pieces of DNA that he has spent several years of his career trying to understand. Dr. Mischel is serving alongside Alice T. Shaw, MD, PhD as chair of the AACR Annual Meeting 2026 Program Committee.
A physician-scientist at Stanford Medicine, Dr. Mischel decided to become a cancer researcher when he was just a teenager, motivated by the loss of his father to stomach cancer. “I promised myself when I was probably 15 years old that I wanted to do something about [cancer],” he recalled.
He spent years pursuing precision oncology to advance the development of treatments that target genetic features specific to a patient’s tumor. But he kept running into the same problem—many patients’ cancers weren’t responding to those targeted therapies.
“These tumors didn’t seem to be following the rules,” he said. “I became convinced that we were missing something big … and was really interested in trying to understand what it was. That’s where our research took us, and we discovered a role for something called extrachromosomal DNA.”
Dr. Mischel explained that extrachromosomal DNAs—or ecDNAs for short—are circular DNA molecules that form when DNA fragments “jump off” chromosomes. The existence of ecDNAs was first reported in 1965, but their role in cancer remained largely unknown until Dr. Mischel and others, empowered by the advent of new technologies, started taking a closer look in recent years.
They discovered that ecDNAs could impact cancer in many ways, influencing its development, progression, and response to treatment. As one example, they found that ecDNAs contain several copies of genes known to drive cancer and harbor features that lead to higher-than-normal expression of those genes.
Moreover, as reported in the AACR journal Cancer Discovery, ecDNAs are unevenly distributed during cell division. This means that instead of each of the two daughter cells receiving the same number of ecDNAs from the dividing cell, as is typical of chromosomal DNA, one of the daughter cells may receive more than the other. This can quickly lead to the accumulation of cancer-promoting ecDNAs with each round of cell division. (Learn more about this study in a post on the AACR blog, Cancer Research Catalyst.)
It can also lead to the rapid accumulation of ecDNAs with gene mutations that confer treatment resistance, said Dr. Mischel. Uneven ecDNA segregation, therefore, “is a path to very rapid resistance,” he noted.
These findings have paved the way for new therapeutic strategies that combat the cancer-driving roles of ecDNA. The furthest along of these takes advantage of the replication stress that occurs on ecDNAs, which makes cell survival dependent on a protein called CHK1. Blocking CHK1 activity killed cancer cells in preclinical studies, and the potential of CHK1 inhibition to treat cancers in patients is now being tested in a clinical trial.
Researchers are also going after ecDNA synthesis, ecDNA segregation during cell division, and ecDNA detection by cellular DNA sensors—highlighting how a basic understanding of ecDNA’s multifaceted roles in cancer is translating to new treatment opportunities.
“We’ve come a long way in understanding the importance of [ecDNA],” said Dr. Mischel. “I’m proud of the fact that we’ve begun to shed real light on this, and that this work, I think, has real promise for making a difference in patients’ lives.”

Researchers are shedding light on the multifaceted ways that extrachromosomal DNA impacts cancer development and resistance to targeted therapies. “Hiding in the nucleus, in...

Launched in 2015, AACR Project GENIE® is powering advances in cancer precision medicine through an international collaboration of top...

Decades of pioneering research led to a first-of-its-kind FDA approval for a new type of immunotherapy—tumor-infiltrating lymphocyte (TIL) therapy....

Preventing cancer and identifying malignancies at the earliest, most treatable stages are key areas of focus for the American...
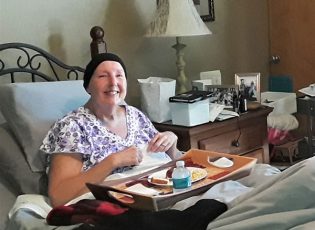
For Margaret McGill, palliative care was key to her cancer care, enabling her to regain her quality of life and reach her goal of undergoing a bone marrow transplant.