Lung Cancer: New Research Brings Good and Bad News
Lung cancer is the number one cause of cancer-related death in the world. In the United States alone, it is expected that 158,080 people will die from the disease this year.
Many researchers are working diligently to help reduce the burden of lung cancer. In the past week, the fruits of the labors of some of these individuals have provided good news for some patients with lung cancer and bad news for those with a stake in lung cancer prevention efforts in the form of new information on the dangers of smoking cigarettes.
New Advances in Cancer Treatment
New research published this week in The New England Journal of Medicine provides good news for the lung cancer community. The study reports that the initial results of the AURA3 phase III clinical trial testing the molecularly targeted therapeutic osimertinib (Tagrisso) as a treatment for certain patients with non–small cell lung cancer (NSCLC) were positive.
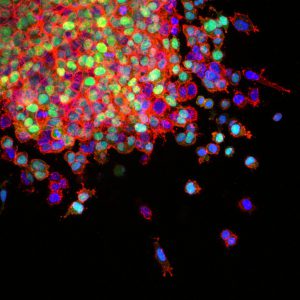
This image shows how lung cancer cells invade surrounding tissues and start to spread (metastasis). Metastatic lung cancer has a poor prognosis; just 4 percent of patients survive five or more years after diagnosis. Image: National Cancer Institute.
As discussed in a previous post on this blog, osimertinib was approved by the U.S. Food and Drug Administration (FDA) in December 2015 for treating patients with NSCLC that has a T790M mutation in the epidermal growth factor receptor (EGFR) gene and that has progressed despite treatment with other EGFR-targeted therapeutics. This approval was based on objective response rate data, rather than overall survival data. As a result, osimertinib’s manufacturer, AstraZeneca, was required by the FDA to conduct a clinical trial to confirm that the drug improves survival for patients.
The data released this week are the first data from that trial and they show that osimertinib significantly increased the time to disease progression compared with standard chemotherapy. Median progression-free survival was 10.1 months for those receiving osimertinib compared with 4.4 months for those receiving standard chemotherapy.
Patients receiving osimertinib through the clinical trial also experienced fewer severe adverse events compared with those receiving standard chemotherapy.
This mirrors the positive experience of Ginger Tam, a 54-year-old single mom with metastatic NSCLC who was featured in the AACR Cancer Progress Report 2016. Ginger received osimertinib through a clinical trial and says about her experience, “Within two months of starting a clinical trial testing a drug called osimertinib (Tagrisso), I had my voice back, along with my breath. Although my lung cancer progressed after two years of receiving osimertinib, my experience with the drug was so awesome that I always said if my lung cancer progressed again, I would look to enroll in a clinical trial testing osimertinib in combination with other treatments.”
Although more time is needed before we can discover whether osimertinib improves overall survival, the new AURA3 data provide more hope for patients with NSCLC, like Ginger.
https://www.youtube.com/watch?v=USJ7YCECBGc
New Insight Into the Dangers of Cigarette Smoking
The Centers for Disease Control and Prevention (CDC) estimate that 90 percent of lung cancer deaths in the United States are attributable to cigarette smoking. What’s more, smoking is responsible for many deaths from 17 other types of cancer as well as numerous additional diseases, such as cardiovascular disease and chronic obstructive pulmonary disease.
The latest data, published last month, show that the percentage of U.S. adults age 18 and older who smoke cigarettes declined from 20.9 percent in 2005 to 15.1 percent in 2015. The data also showed that the proportion of daily smokers declined over the same period, falling from 16.9 percent in 2005 to 11.4 percent 2015.
Despite this progress, research published this week in JAMA Internal Medicine identified new concerns about the health consequences of cigarette smoking. The results showed that even low-intensity smoking—defined as less than one (but more than zero) or 1–10 cigarettes a day—over a long period of time was associated with a significantly increased risk of death from any cause, including death from lung cancer and cardiovascular disease.
The data led the authors to conclude, “These findings provide further evidence that there is no safe level of cigarette smoking. All smokers should be targeted for smoking cessation, regardless of how few cigarettes they smoke per day.”

Another area of concern highlighted by a second study published this week in JAMA Internal Medicine is the tremendous disparity in smoking-related cancer deaths that exists in the United States. In this study, the researchers found that although the proportion of cancer deaths attributable to cigarette smoking varied substantially across states, the majority of states with the highest proportion of cancer deaths attributable to cigarette smoking were in the South.
The authors note, “Higher SACM [cigarette smoking–attributable cancer mortality] in the South is driven by higher historic smoking prevalence, which has prevailed in large part due to weaker tobacco control policies and programs.”
In an accompanying commentary, three leading researchers expand on this idea by providing information on cancer control policies and programs in the 10 states with the highest and lowest rates of cigarette smoking–attributable cancer mortality. They conclude that there are “weaker policy environments in the 10 states with the highest rate—substantially lower cigarette excise taxes, no comprehensive smoke-free policies, triple the rate of preemption of tobacco control policies, and modest program spending.”
In sum, the new research into the health consequences of cigarette smoking points to the need for concerted efforts to further promote tobacco control and cessation policies and programs throughout the United States. Through its Tobacco and Cancer Subcommittee, the American Association for Cancer Research (AACR) is committed to fostering scientific and policy initiatives to reduce the incidence of disease and mortality due to tobacco use. This is just one approach by which the AACR is working to support research designed to accelerate the pace of progress in lung cancer prevention and treatment.



