The Past, Present, and Future of HPV: Can Vaccination Help Eliminate Cervical Cancer?
On a web page titled “14 Diseases You Almost Forgot About (Thanks to Vaccines),” the Centers for Disease Control (CDC) remind us that the United States has eliminated or drastically reduced cases of several diseases—such as polio, measles, and diphtheria—due to widespread vaccination programs. The COVID-19 pandemic is serving as a real-time lesson about the role of vaccination in preventing infectious diseases, but in the shadow of this rapid eradication effort, a different vaccine is slowly driving the decline of a different virus known to cause several cancers.
Human papillomaviruses (HPV) are a group of sexually transmitted infections, some of which can increase the risk of cervical, anal, penile, vaginal, vulvar, and oropharyngeal cancers. Vaccines against HPV became available in 2006, and as the first adolescents who received the vaccine age, the incidence of these cancers is expected to decrease. Some experts believe that cervical cancer, which is associated with HPV in more than 90 percent of cases, could be virtually eliminated in the coming decades.
Because the current standard-of-care vaccine is over 90 percent effective at preventing infection by nine HPV types, seven of which are known to cause cancer, high vaccination rates could drive cervical cancer incidence below the threshold of near-elimination, which the World Health Organization (WHO) defines as fewer than four cases per 100,000 people. The vaccine is currently recommended for all adolescents aged 9 to 15, with catch-up regimens available up to age 26 or, in some cases, age 45.
HPV is extremely prevalent in the adult population, and prior to vaccine availability, nearly everyone was expected to become infected over the course of their lifetime. The immune system clears the vast majority of HPV cases within a couple of years, but if the infection persists longer, it can change the morphology of infected cells, resulting in a lesion that may develop into cancer.
For Gynecologic Cancer Awareness Month, we provide a recap of HPV’s role in the way researchers view cervical cancer, a look forward at cervical cancer elimination projections, and a discussion of how other factors, such as health disparities, may hinder progress.
The Journey Toward Elimination
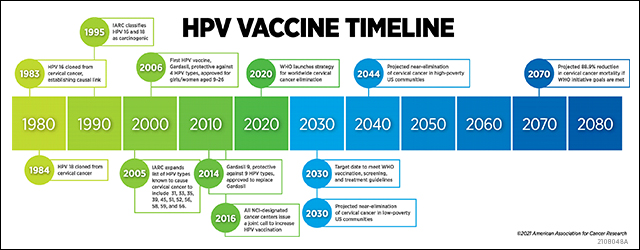
In the early 1980s, scientists had only identified a few mechanisms underlying cancer development, and infection with viruses—such as the Epstein-Barr virus and hepatitis B virus—was one of them. Harald zur Hausen, MD, FAACR, and colleagues successfully cloned HPV 16, one of the most carcinogenic HPV types, from a cervical cancer sample in 1983 and followed it up with the cloning of HPV 18 from another cervical cancer sample a year later. For this groundbreaking work, zur Hausen was awarded the Nobel Prize in Medicine or Physiology in 2008.
Despite these advances, however, HPV 16 and 18 weren’t officially classified as carcinogens until 1995, when the International Agency for Research on Cancer (IARC) published a monograph about human papillomaviruses, in which they reviewed over 100 case-controlled and cohort studies of cervical cancer and cancers from other sites. They concluded that HPV 16 and 18 were carcinogenic to humans; HPV 31 and 33 were probably carcinogenic to humans; and several other HPV types were possibly carcinogenic to humans.
The large number of cancer cases believed to be caused by these viruses spurred an effort to develop a vaccine. In 2006, the U.S. Food and Drug Administration (FDA) approved Gardasil, which protected against HPV 16 and 18, as well as HPV 6 and 11, the most common drivers of genital warts. Because prevention against HPV infection is most protective before an individual becomes sexually active, the vaccine was approved for girls and women aged 9 to 26. In 2009, the FDA expanded this approval to include boys and men of the same age group, in order to decrease HPV transmission and improve protection against anal, penile, and oropharyngeal cancers.
In 2007, however, IARC published a follow-up monograph, assembled by a working group convened in 2005, updating the data on HPV structure, transmission, infectivity, and its relationship to cancer. This working group expanded the list of carcinogenic HPV types to include HPV 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, and 66. Although HPV 16 and 18 remained the most common types tied to HPV-driven cancers, this expansion prompted research toward a new vaccine with more comprehensive protection. In 2014, the FDA approved Gardasil 9—a new Gardasil vaccine that protected against the four types included in the previous version, plus HPV 31, 33, 45, 52, and 58—for women and girls. Approval was expanded to include men and boys in 2015.
Despite the efficacy of the HPV vaccine, issues with vaccine availability and hesitancy have hindered its overall effect. In 2015, a CDC report estimated that only 40 percent of girls and 21 percent of boys had received all three recommended doses of the vaccine. To address these low rates, all 69 NCI-designated cancer centers issued a joint call to action in 2016, with the goal of increasing HPV vaccination rates.
Following this show of support, vaccination uptake has improved—an estimated 50 percent of girls and 30 percent of boys aged 11-17 have now completed the vaccination series, and nearly 70 percent of girls and 50 percent of boys have initiated it. These numbers fall short of the Office of Disease Prevention and Health Promotion’s Healthy People 2020 vaccination target of 80 percent, but many scientists agree that these efforts will push cervical cancer cases below the near-elimination threshold in the coming decades. Due to health care inequities, however, not all areas are scheduled to reach this milestone at the same time.
Health Disparities and Cervical Cancer Elimination
Disparities in insurance coverage, cancer screening, access to treatment, and other social determinants of health have created significant differences in outcomes between cancer patients of different races, ethnicities, and socioeconomic status. Cervical cancer is no exception—according to the 2020 AACR Cancer Disparities Progress Report, HPV infections are more prevalent among African Americans aged 18 to 59 than their white or Hispanic counterparts, and African American and Hispanic women have higher rates of HPV-related cervical cancer than other racial and ethnic groups. How do these factors affect the path toward cervical cancer elimination in the U.S.?
A recent study published in Cancer Epidemiology, Biomarkers & Prevention investigated how the cervical cancer elimination timeline might differ between high-poverty and low-poverty communities. As the first adolescents who received the HPV vaccine are only beginning to enter the age range where cervical cancer is prominent, researchers have relied on statistical modeling to predict how vaccination will impact cervical cancer incidence in the coming years. In this study, Jennifer Spencer, PhD, an assistant professor at the University of Texas at Austin, who performed this work as a research fellow at the Harvard School of Public Health, and her colleagues assembled a series of models based on current data from counties in the highest and lowest quartile of poverty in the U.S.
They integrated information about the risk of HPV transmission among vaccinated and unvaccinated individuals, the probability of HPV progressing to cervical cancer, the rates of cervical cancer screening, and the odds of effective cancer treatment to simulate two hypothetical counties—a high-poverty county and a low-poverty county. They modeled how these parameters would affect cervical cancer incidence through the year 2070 and found that low-poverty communities could reach near-elimination by 2030, but that high-poverty communities wouldn’t meet that goal until 2044.
According to Spencer, this disparity didn’t appear to result from differences in vaccination rates between low- and high-poverty areas, but rather from disparities in cervical cancer screening and a significant difference in the types of HPV commonly found in these communities. In high-poverty areas, researchers found that approximately 18.3 percent of HPV infections were caused by types the vaccine doesn’t protect against, compared to 8.9 percent in low-poverty areas.
Although this study didn’t identify differences in vaccine coverage between individuals in low- and high-poverty areas, racial and geographical vaccination disparities still persist. According to the 2020 AACR Cancer Disparities Progress Report, African American girls aged 13 to 17 are less likely to have received a full HPV vaccine regimen than white girls. Data from the 2020 National Immunization Survey—Teen (NIS-Teen) also showed stark differences in coverage by state, with an estimated 79.9 percent of Rhode Island girls aged 13 to 17 up to date on their HPV vaccines, compared with only 32.6 percent in Alabama. The elimination timelines outlined in the study by Spencer and colleagues depend on vaccination rates of approximately 70 percent.
Results from a 2018 study in JAMA Pediatrics suggest that health care providers may be a productive point of intervention to increase HPV vaccination. In this study, the researchers introduced physicians at eight primary care practices to a five-step communication strategy aimed at increasing HPV vaccination. The intervention consisted of a fact sheet library that practices could tailor to their needs, an informational website to which practices could refer parents, a library of images depicting HPV-driven diseases, a vaccination decision aid, and a 2.5-hour communication seminar to strengthen physicians’ communication with patients and parents about the vaccine.
Patients at practices that received the intervention were 1.46 times more likely to initiate the HPV vaccine series and 1.56 times more likely to complete the series, as compared to control practices that did not receive the intervention. Further, the researchers suggest that the intervention is sustainable long-term, as 98 percent of physicians in the intervention group said they’d likely continue using the fact sheets and 91 percent said they’d likely continue using the communication techniques.
While this study was localized to practices around the Denver area, it suggests that such interventions may be useful in areas and among populations with low HPV vaccination rates nationwide. Vaccination disparities, however, do not exist exclusively within the United States. As with other infectious diseases, the quest for elimination requires an international perspective, and scientists worldwide are working to address this issue globally.
Cervical Cancer Elimination Worldwide
In 2020, the WHO launched the Cervical Cancer Elimination Initiative—a global call to action to eliminate cervical cancer worldwide by increasing rates of vaccination, screening, and cervical cancer treatment. They suggest that, in order to reach near-elimination of cervical cancer by the end of the century, all countries will need to meet these three milestones by 2030:
- vaccinate 90 percent of girls by age 15
- screen 70 percent of women for HPV infection by age 35 and again by age 45, and
- deliver adequate treatment to 90 percent of cervical cancer patients.
A recent study in Cancer underscores the challenges associated with achieving this goal, especially in low- and middle-income countries. In this study, the researchers correlated cervical cancer incidence and mortality with the Human Development Index (HDI)—a measure of national socioeconomic development—for 31 countries. They found that both incidence and mortality were inversely related to a country’s HDI value, meaning that poorer countries faced a disproportionately high cervical cancer burden. Further, the study found that incidence and mortality of cervical cancer decreased or remained stable for the vast majority of countries between 2007 and 2017, which can help epidemiologists identify intervention strategies that are working in these countries, or gaps that are present in countries with increasing rates.
A 2020 study in Lancet provided hope that reaching the goals outlined by the WHO would decrease these disparities and propel cervical cancer toward worldwide elimination. The authors of this study developed models to predict how cervical cancer incidence and mortality would change in low- and middle-income countries if the WHO elimination goals were met by 2030.
The models predicted that achieving all three WHO cervical cancer elimination goals by 2030 would result in an 88.9 percent decrease in cervical cancer mortality by 2070 and a 98.6 percent decrease by 2120. Reaching the 90 percent vaccination target alone, in the absence of the screening and treatment targets, would decrease mortality by 61.7 percent by 2070 and by 89.5 percent by 2120.
These data suggest that, as a global society, we can make robust changes in cervical cancer incidence and mortality in the coming decades. While vaccination is a crucial component of this process, it is not the only consideration; near-elimination could be significantly delayed in the absence of improved access to screening and treatment.