FDA Approves New Lung Cancer Treatment and First Next-Gen Companion Diagnostic
Recent decisions by the U.S. Food and Drug Administration (FDA) are significantly advancing the field of precision medicine.
Hot on the heels of the FDA’s landmark approval of an anticancer immunotherapeutic for use based on whether a patient has a tumor with certain biomarkers, rather than a tumor originating at a certain anatomic site, the agency approved the first companion diagnostic that can detect mutations in multiple genes in a single test.
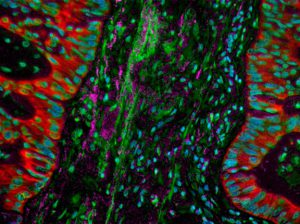
Lung cancer is the second most commonly diagnosed cancer in the United States. As shown here, lung cancer is associated with a vast stromal desmoplastic reaction in which the connective tissue, associated with the tumor, thickens similarly to scars. Image courtesy of the National Cancer Institute.
The ability to screen a single lung cancer tissue sample for mutations that predict likely response to three different treatment options, rather than having to screen samples one mutation at a time, has the potential to expedite the selection of the right targeted therapy for the patient.
What is precision medicine?
Precision medicine, which is sometimes referred to as personalized medicine, molecular medicine, or tailored therapy, is broadly defined as treating a patient based on characteristics that distinguish that person from other patients with the same disease.
Currently, the presence of certain molecular or genetic features in a patient’s tumor is the main factor influencing precision medicine in oncology. This is because several decades of research have led to the accumulation of a deep understanding of the genetic mutations that lead to cancer initiation, development, and progression. Alongside this growing knowledge has been the development of therapeutics targeted to the specific molecules affected by the mutations.
The effective use of therapeutics targeting particular cancer-driving molecular abnormalities often requires tests called companion diagnostics. The tests detect the presence of particular genetic mutations or molecular abnormalities in a patient’s tumor so that he or she can receive treatment with the matched molecularly targeted therapeutic.
As we increase our understanding of other biological characteristics that influence the course of cancer and its response to treatment, including a patient’s genome, lifestyle, and microbiome, and increase our ability to analyze these in the way that we analyze cancer genomics data, we can expect faster and broader implementation of precision medicine.
The latest in precision medicine for lung cancer patients
Non–small cell lung cancer (NSCLC) is the most common type of lung cancer diagnosed in the United States. In fact, it is estimated to account for 84 percent of lung cancer cases, which translates into 186,900 new cases expected to be diagnosed in 2017.
NSCLC is also one of the types of cancer that has been at the forefront of the implementation of precision medicine in oncology because research provided extensive insight into the genetic mutations that fuel NSCLC growth in certain subgroups of patients and led to the development of therapeutics that target the effects of these mutations.
The most recent advance occurred last week, when the FDA approved the use of a combination of molecularly targeted therapeutics, dabrafenib (Tafinlar) and trametinib (Mekinist), for the treatment of NSCLC harboring a specific mutation in the BRAF gene, BRAF V600E.
The BRAF V600E mutation is detected in 1 to 2 percent of NSCLCs. According to the FDA, the approval of the combination of dabrafenib, which targets the abnormal BRAF V600E protein, and trametinib, which targets two other proteins—MEK1 and MEK2—that function in the same signaling network as BRAF V600E, was based on results from the Study BRF113928 phase II clinical trial. Among 93 patients with NSCLC that tested positive for the BRAF V600E mutation who were treated with the dabrafenib/trametinib combination, 61 percent had tumor shrinkage.
Alongside this approval, the FDA also approved a companion diagnostic to identify patients eligible for the new combination treatment, those who have NSCLC with a BRAF V600E mutation. The new companion diagnostic, Oncomine Dx Target Test, is the first FDA-approved companion diagnostic to use next-generation sequencing technology. Through the use of this technology, a single test can provide information on not just one gene but on a panel of 23 genes. In addition to being able to detect the BRAF V600E mutation, the Oncomine Dx Target Test can simultaneously assess for the presence of mutations in the EGFR and ROS1 genes that indicate treatment with the FDA-approved molecularly targeted therapeutics gefitinib (Iressa) and crizotinib (Xalkori), respectively. Thus, it is the first companion diagnostic approved for use in matching patients to any one of multiple molecularly targeted therapeutics.
According to the company that makes the Oncomine Dx Target Test, ThermoFisher Scientific, many of the other genes that this test provides information on are being investigated as potential biomarkers for molecularly targeted therapeutics. Thus, it is possible that the utility of the Oncomine Dx Target Test will expand in the future.